Dr. Kugathasan’s research goal is to further extend novel genetic discoveries in inflammatory bowel disease (IBD), in particular common and rare susceptibility variants that are the cause of very early onset IBD. In addition, he has been investigating the immunogenetic mechanisms that underlie this chronic intestinal inflammation in children and adults with IBD. He is the principal investigator of a large 40 site, multicenter research network where thousands of incident cases of early onset IBD are being enrolled. DNA, plasma and intestinal biopsy materials are being banked to identify modifier genes, environmental, and microbial factors that can be used to stratify the risk of complicated disease and surgery in IBD. As a clinician and an inflammatory bowel disease specialist, he also serves as scientific director of the inflammatory bowel disease program at Children’s Health Care of Atlanta and sees pediatric patients with inflammatory bowel disease, (both Crohn’s disease and ulcerative colitis) at Emory Children’s Center and Egleston Children’s hospital.
Dr. Kugathasan received his medical degree from Sri Lanka. After pediatric residency in Sinai Hospital of Baltimore, he completed his pediatric gastroenterology fellowship at Case Western Reserve University. His research training was in mucosal immunology under the mentorship of Dr. Claudio Fiocchi. In 2002, he received the Physician of the year award from Crohn’s and Colitis Foundation of America. He was the recipient of the prestigious young clinical investigator award from the society of North American Pediatric Gastrenterology & Nutrition (NASPGHAN) and junior physician investigator award from American Federation for Medical Research (AFMR). He has served as a co-chair for pediatric affairs of Crohn’s and Colitis foundation of America. He moved to Emory University in 2008, and has been appointed as a Marcus Professor of Pediatric Gastroenterology / Inflammatory bowel disease. Outside of work Subra enjoys travelling, spending time with family, and tending to his backyard garden.
The Kugathasan research team (IBD Dream Team) focuses on early onset Inflammatory Bowel Disease (IBD). Inflammatory bowel disease (IBD), which includes Crohn’s disease (CD) and ulcerative colitis (UC), is estimated to affect approximately 1.2 million Americans. IBD is a destructive, life-long, chronic inflammatory disorder which results in gastrointestinal bleeding, weight loss and poor quality of life. IBD affects all races and onset of the disease is usually in children and young adults. Familial, twin and linkage studies suggest that CD is highly heritable. The research interest of the laboratory are:
 |
To determine and identify genetic associations in very young onset IBD in comparison to those found in older patients with adult onset disease. In particular, to identify high effect, highly penetrant but rare variants that cannot be identified by genome wide association studies. |
 |
To identify susceptibility and modifying factors and perform Genotype – serotype – bacteriotype - gene expression studies in carefully and prospectively identified incident cases of early onset IBD. |
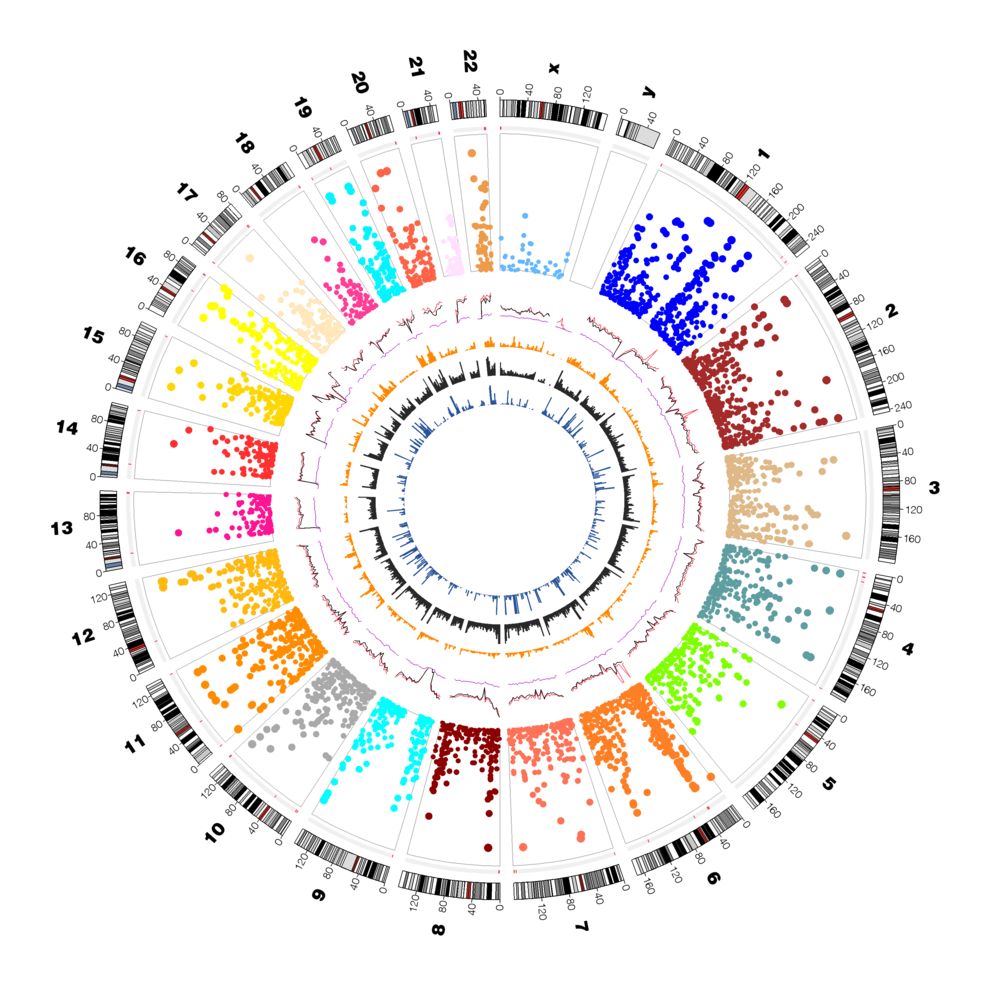 |
Genome wide association studies to determine common SNPs / loci and copy number variants in African Americans with IBD. Replication studies in African Americans show that the major genetic variants that were found in Caucasians with IBD are not associated with African Americans. |
 |
Use of the latest generation sequencing technologies to comprehensively identify IBD - predisposing causal variants in order to fully characterize the physical scale of various genetic associations in IBD. Performing targeted sequencing in susceptibility loci found in African Americans and Caucasians in parallel is another area of interest. |
 |
Development of patient derived intestinal enteroids and colonoids which are miniaturized intestines produced from the patients own biopsy specimen. To do this we obtain biopsy specimens from patients undergoing a routine colonoscopy at Children's Healthcare of Atlanta Egleston and Emory Univeristy Hospital. The goal of this project is twofold: to establish a large diverse enteroid / colonoid biobank, which will be a valuble resource for researchers in the near future; and to screen individual patients for drug response, which could dramatically change the way drugs are prescribed to patients in the future bringing us closer to our goal of personalized medicine. |
The Kugathasan Research Team has many projects that are currently being worked on. Funding from multiple sources including government and private foundations ensures we are able to keep doing group breaking research. The current research projects are below:
RISK Stratification:
Pediatric onset CD is the fastest growing incident age group as is considered to be a more aggressive phenotype than adult onset disease. At presentation, the most of the children present with an inflammatory or so called non-complicated disease behavior. Over time a sub-group of CD patients progress to more a complicated disease behavior, which involve hospitalization and sometimes surgery. The factors or pathogenic mechanisms underlying the development of complications are poorly understood. Therefore, discovery of predictive factors contributing to the progression of a CD patient from an uncomplicated to complicated phenotype necessitates engaging a patient population naïve to all therapies and devoid of any confounding factors. In 2008 the RISK (Risk Stratification and Identification of Immunogenetic and Microbial Markers of Rapid Disease Progression in Children with Crohn’s Disease) study was commenced at 28 investigative centers in North America with the goal of prospectively characterizing and predicting the natural history of newly diagnosed CD in children presenting with uncomplicated disease.
To this end, over 1000 CD patients have been prospectively enrolled at this study. Each patient was followed for over 5 years. All patients were required to undergo a baseline colonoscopy before treatment with findings recorded in a standardized fashion. At enrollment and during ongoing prospective follow-up evaluation, medication exposure, clinical, radiological, endoscopic and laboratory data were obtained for each enrolled patient and submitted to a centralized data management center. All patients were managed according to the dictates of their physicians, not by standardized protocols. The institutional review board of each site reviewed and approved the protocol and each participant provided written informed consent. Blood for genomic DNA, serology, stool and biopsy samples were collected at the time of diagnosis in all subjects. Patients were followed up at minimum of every 6 months. During the follow up visits for up to 3 years, blood samples and (on occasion) ileal biopsy were collected. Currently our team is working towards the primary aim of the project, which is to develop a composite risk score using phenotypes, genetics, serology, microbiome and gene expression markers.
Funding provided by Crohn’s and Colitis Foundation of America (CCFA)
Gene Discoveries in Subjects with Crohn’s Disease of African Descent (Genesis AA Study):
Nearly all genetic studies of IBD are focused on Caucasians; however, there is emerging data suggesting that the disease burden is similar in African Americans (AA). Variation data from HapMap, 1000 Genomics, and other disease studies suggests that the allelic architecture of AA populations could be significantly different from Caucasians. A large sample size is needed for an adequately powered genetic study. Additionally, the AA population has much more genetic variation. We are currently in alliance with the NIDDK IBD Genetics Consortium’s (IBDGC) mission to dramatically increase the recruitment of AA patients (pediatric and adult) IBD subjects for gene discovery purposes.
Funding provided by National Institutes of Health (NIH/NIDDK) R01DK087694
DNA Methylation / Epigenetics
Epigenetic modifications induce changes in gene expression through structural alterations of DNA that are maintained through each round of cell division; they respond to changes in the environment, are potentially reversible and can be targeted for disease therapies. DNA methylation at cytosine-guanine dinucleotides (CpG sites) is the epigenetic modification that is most commonly studied in humans. It regulates gene expression by influencing the recruitment and binding of regulatory proteins to DNA. Typically, an increase in methylation at gene promoter regions correlates with a decrease in expression of that gene Intragenic DNA methylation is also important to regulate alternative promoters and enhancers that define a variety of alternative transcripts.
- Aim 1: Characterize DNA methylation differences over the course of treatment in pediatric Crohn’s cases over 3 years of treatment.
- Aim 2: Characterize epigenetic markers in intestinal tissue to assess the utility of both whole blood and intestinal methylation patterns as biomarkers to predict side effects following treatment.
Funding provided by National Institutes of Health (NIH/NIDDK) R21DK119997
Leveraging gene dropout patterns in single-cell RNA-seq to identify novel cell types in the ileum of patients with Crohn's disease
We will use this cohort to evaluate and validate the utility of dropout-based computational methods for single-cell RNA-seq analysis in the context of Crohn’s disease (CD). Crohn’s disease is a chronic inflammatory disease, characterized by remitting relapsing inflammation affecting transmurally – that is, the inflammation goes beyond the mucosa, necessitating mapping of epithelial cells along with the immune and non-immune cells of the lamina propria to observe the complete picture. We will obtain colonoscopically pinch mucosal biopsies from CD and controls, as this provides the needed cells from mucosa and sub-mucosa. Although CD can affect any part of the gut, terminal ileum biopsies are proposed here, because the ileum is involved in 70% or more of subjects with CD. Since the status of active inflammation can greatly influence the transcriptomic profiles of each cell type in the gut, an ideal experiment should include samples representing the active stage (inflamed), inactive stage (non-inflamed), and compared with non-disease normal control. We also aim to explore racial and ethnic contributions to variability in scRNA-seq in the gut pertaining to CD pathology.
-
Aim 1: Generate scRNA-seq data from Crohn’s patients using gut tissue.
-
Aim 2: Apply and compare co-occurrence clustering and Seurat to the scRNA-seq data.
-
Aim 3: Compare the heterogeneity across the three proposed sample groups.
Funding provided by The Leona M. and Harry B. Helmsley Charitable Trust
The Kugathasan Research Team has many clinical trials that patients are actively being recruited for. These studies are used to better understand how IBD affects patients and provides a mechanism for patients to actively participate in research. The current clinical trials are below:
Develop - A Multi-center, Prospective, Long-term, Observational Registry of Pediatric Patients with Inflammatory Bowel Disease. The purpose of this study is to collect long-term safety information on the disease and medications that you received or are receiving for your inflammatory bowel disease.
Cape Registry - A long-term (10 years) post-marketing observational study to assess the safety and effectiveness of Humira (Adalimumab) in pediatrics with moderately to severely active Crohn’s Disease.
MSC Infusion (No more recruitment) – In this Phase 1 trial, the investigators intend to show safety and tolerability of autologous MSC, expanded using a non-xenogeneic, human component platelet lysate expansion media. Fresh, non-cryopreserved, autologous MSCs will be delivered intravenously as a single bolus dose in a dose-escalation phase I study. The investigators intend to test whether the product is clinically safe in adults (18-65 years old) with CD and to determine the maximal deliverable dose. The secondary endpoint will monitor effectiveness using CDAI as an endpoint.
Biomarkers of Intestinal Fibrosis in Small Bowel Crohn's Disease - The primary purpose of this study is to test whether a cadre of novel blood and MRI biomarkers can distinguish fibrotic from non-fibrotic CD lesions, either individually or in combination. This will be achieved by comparing the biomarker results of stricturing CD patients undergoing small bowel resection (AIM 1) to the results of CD patients with inflammatory non-stricturing, non-penetrating lesions (AIM 2). Secondary purposes of this study are 1) to establish normative values for the novel blood-based biomarkers in healthy volunteer subjects without known bowel inflammation, and 2) to characterize and compare the fecal calprotectin and microbiota in small bowel CD patients with B1 and B2 or B3 disease as well as healthy volunteer subjects.
Mechanisms of Intestinal Inflammation following Heal Resection for Crohn's Disease: Building a biobank of data and samples to build a predictive model of disease recurrence (Ileal Post-Op Study) - The objective of this study is to identify the genetic, serological and microbial factors associated with the recurrence of inflammation following ileal resection for Crohn’s Disease (CD). This study will also investigate mechanistic pathways in disease pathogenesis.
Relation of Social Factors with Racial Disparities in Pediatric Inflammatory Bowel Disease (SaFR kids)
If interested please email ibdresearch@emory.edu for more information
Associate Director, Research Projects
| To Be Determined |
|---|
Clinical Research Coordinators
 |
Chantrice Rogers, MPH Clinical Research Coordinator Chantrice joined the Kugathasan lab in August of 2015. She is a graduate of Savannah State University and has a Masters Degree in Public Health from Mercer University. Chantrice is one of our Clincial Research Coordinators and she manages various research trials within the group. When she is not in the office, you may find her volunteering or planning her next global excursion. |
|
|
Bernadette Martineau MS, RD Clinical Nutritionist / Clinical Research Coordinator Bernadette joined the Kugathasan lab in December of 2012. She is a graduate of Georgia State University with a MS in nutrition. She is the clinical nutritionist in the IBD clinic and also helps to consent and collect patient samples for research. When she is not in clinic, you might find her driving her two dogs around in her dog taxi or hiking with her husband and two dogs. She also loves cooking and trying out new recipes. |
|
|
Nia King, MS Clinical Research Coordinator Nia joined the Kugathasan lab in November of 2019. She is a graduate of Spelman College and has a Master’s Degree in Medical Physiology from Case Western Reserve University. Nia is a Clinical Research Coordinator and she oversees different research trials; as well as collects patients’ samples. When she is not working, she is typically hiking, listening to music, or reading a good book. |
Laboratory Research Team
 |
Anne Dodd Laboratory Manager Anne joined the Kugathasan lab in April of 2016. She is a graduate of Appalachian State University. Anne oversees the day to day operations of the Kugathasan lab. In her spare time you can find her enjoying all the outdoors has to offer, along with her three dogs. |
 |
Suresh Venkateswaran, PhD Research Associate Suresh joined the Kugathasan lab in September 2015. He recieved his PhD in Bioinformatics from Bharathidasan University inTamilnadu, India. Currently, he is involved in data mining projects from Genotyping, Exome sequencing, Whole genome sequencing, Transcriptomic (RNASeq), Microbiome and DNAmethylation. His hobbies are cooking traditional south Indian food, travelling, playing board games and driving. |
.JPG) |
Jason D. Matthews, PhD Assistant Professor Dr. Matthews joined the Kugathasan IBD Dream Team in 2019. He graduated from Georgia State University in 2010 with a doctorate degree in Genetics and Biochemistry, with a focus on molecular virology. He has advanced postdoctoral training in mucosal biology of the intestine and microbiome, is an expert in molecular cell biology and microscopic imaging, and focuses on unraveling the molecular basis of inflammatory bowel disease. He oversees research projects that include the use of intestinal epithelial organoids, single-cell RNA sequencing and spatial transcriptomics. |
 |
Information Analyst
|
 |
David Hercules Data Analyst David joined the Kugathasan lab in June 2019. He graduated from Emory University with a Chemistry BS in 2017. David is the database manager for over 5 clinical research studies, assisting researchers and research coordinators across the US and abroad with data requests, data analysis and visualization, and data entry and cleaning help. When he is not looking at spreadsheets, he likes to play soccer, take a dip in the pool, eat spicy food, and hang out with friends. |
 |
Ranjit Pelia Laboratory Technician Alumni of Emory University, B.S. in Anthropology & Biology, and Oxford College. Currently engaged in clinical pediatric research focused on unraveling epigenetic interplays involved with Inflammatory Bowel Disease at Emory University. Duties involve serving as a Clinical Research Coordinator, CRC, and lab technician for biological specimens assaying, processing, and maintaining the biobank repository of Kugathasan Lab. Also a candidate for MPH in Global Environmental Health at Rollins School of Public Health. Research involves a better understanding of epigenetic modulation of non-coding RNAs in IBD. |
Current Clinical Fellow
 |
Duke Geem, MD, PhD Clinical Fellow Duke joined the Kugathasan lab in July of 2020. He completed the Medical Scientist Training Program at Emory University School of Medicine (SOM) and obtained his PhD under the mentorship of Dr. Tim Denning in mucosal immunology investigating the regulation of intestinal CD4+ T cells by antigen-presenting cells and working with animal models of IBD. He completed his Pediatric Residency at the University of California San Francisco and returned back to Children’s Healthcare of Atlanta/Emory SOM to complete his Pediatric Gastroenterology, Hepatology, and Nutrition Fellowship on the Accelerated Research Pathway. His clinical interest is in Pediatric and VEO IBD, and his research interests are in understanding the immune mechanisms by which pediatric patients with IBD stop responding to treatment with the ultimate goal of developing novel cellular and molecular therapies. When Duke is not in the hospital or lab, he enjoys cycling, spending time with his family, reading research articles, and catching up on sleep. |
Trainees
 |
Murugadas Anbazhagan, PhD Post Doc Murugadas joined the Kugathasan lab in March of 2020. He received his PhD in Environmental Biotechnology from Bharathidasan University in Tamil Nadu, India. His current research interests are primarily focused on the generation of Patient-Derived Organoids (PDOs) as a novel platform to dissect Inflammatory Bowel Disease. In his free time, Murugadas enjoys playing cricket and badminton, reading novels, and watching movies. |
Past Clinical Fellows
 |
Rebecca Scheer, MD |
 |
Clifton Huang, MD |
 |
Jeremy Middleton, MD |
 |
Robert Simek, MD |
 |
Tatyana Hofmekler, MD |
 |
Sana Syed, MD |
 |
Jordan Weitzner, MD |
 |
Cortney Ballengee, MD |
Past Medical Student Trainees
Madeline Bertha, MD
Hillary Shapiro, MD
Shiva Shirazi, MD
Oloruntosin Adeyanju, MD
Please see a few of the recent publications that have originated directly from our research group
Names in BOLD denotes members of the Kugathasan Lab
2017
2016
2015
2014
2013
People2People Researchers make Crohn's Disease discovery
Genome study identifies risk genes in African Americans with inflammatory bowel disease
Study describes genetic risks for inflammatory bowel disease in African-Americans
People2People CCFA Channel 2 News
NIH Awards Emory $4.8 Million to Study Genetics of Crohn's in African Americans
Emory Awarded $5 Million to Study Crohn's Disease in Children
Crohn's disease study uses patients' own bone marrow cells for personalized treatment


